Infiltrative Basal Cell Carcinoma with Nodal Metastasis in a 74-year-old Female
A Case Report
DOI:
https://doi.org/10.21141/PJP.2025.01Keywords:
basal cell carcinoma, X-ray, squamous cell carcinoma in-situ, infiltrative basal cell carcinoma, basaloid cellsAbstract
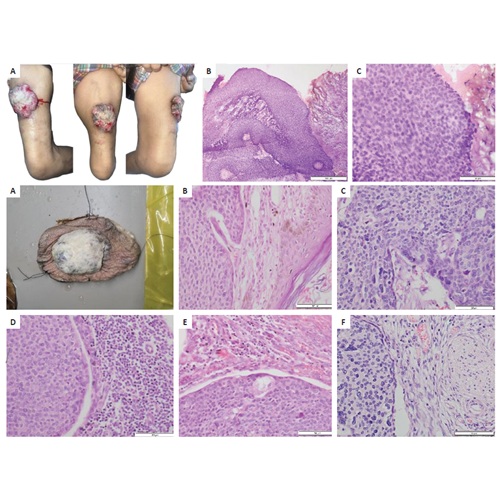
Basal cell carcinoma, the most common human malignancy, has a rare incidence of metastases ranging from 0.0028-0.55%. We report a case of a 74-year-old female with a 10-year history of an enlarging anterior thigh nodule. Wide resection and inguinal lymph node dissection revealed an infiltrative basal cell carcinoma with lymph node metastasis due to the presence of basaloid cells, limited peripheral palisading, loose stroma, extensive spread, perineural invasion and immunoreactivity to p40, BerEP4, and GATA3.'
Downloads
References
Lomas A, Leonardi-Bee J, Bath-Hextall F. A systematic review of worldwide incidence of nonmelanoma skin cancer. Br J Dermatol. 2012;166(5):1069-80. https://pubmed.ncbi.nlm.nih.gov/22251204 https://doi.org/10.1111/j.1365-2133.2012.10830.x DOI: https://doi.org/10.1111/j.1365-2133.2012.10830.x
WHO Classification of Tumors Editorial Board. Skin tumors. Lyon (France): International Agency for Research on Cancer; 2023. WHO Classification of Tumors Series, 5th ed. vol. 12.
Dika E, Scarfì F, Ferracin M, et al. Basal cell carcinoma: a comprehensive review. Int J Mol Sci. 2020;21(15):5572. https://pubmed.ncbi.nlm.nih.gov/32759706 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7432343 https://doi.org/10.3390/ijms21155572 DOI: https://doi.org/10.3390/ijms21155572
Takahashi C, Kanazawa N, Yoshikawa Y, et al. Germline PTCH1 mutations in Japanese basal cell nevus syndrome patients. J Hum Genet. 2009;54(7):403-8. https://pubmed.ncbi.nlm.nih.gov/19557015 https://doi.org/10.1038/jhg.2009.55 DOI: https://doi.org/10.1038/jhg.2009.55
Chitta S, Patel J, Renapurkar S, et al. Nevoid basal cell carcinoma syndrome: a case report and literature review. Ophthalmic Genet. 2022;43(1):27-35. https://pubmed.ncbi.nlm.nih.gov/34608840 https://doi.org/10.1080/13816810.2021.1983847 DOI: https://doi.org/10.1080/13816810.2021.1983847
Ferrucci LM, Cartmel B, Molinaro AM, et al. Host phenotype characteristics and MC1R in relation to early-onset basal cell carcinoma. J Invest Dermatol. 2012;132(4):1272-9. https://pubmed.ncbi.nlm.nih.gov/22158557 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC3305835 https://doi.org/10.1038/jid.2011.402 DOI: https://doi.org/10.1038/jid.2011.402
Pellegrini C, Maturo MG, Di Nardo L, Ciciarelli V, Gutiérrez García-Rodrigo C, Fargnoli MC. Understanding the molecular genetics of basal cell carcinoma. Int J Mol Sci. 2017;18(11):2485. https://pubmed.ncbi.nlm.nih.gov/29165358 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5713451 https://doi.org/10.3390/ijms18112485 DOI: https://doi.org/10.3390/ijms18112485
Wahl RU, Cacchi C, Rübben A. Cutaneous basal cell carcinoma with lymph node and pulmonary metastases. Case Rep Oncol Med. 2018;2018:3485326. https://pubmed.ncbi.nlm.nih.gov/29854516 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5941720 https://doi.org/10.1155/2018/3485326 DOI: https://doi.org/10.1155/2018/3485326
Laga AC, Schaefer IM, Sholl LM, French CA, Hanna J. Metastatic basal cell carcinoma. Am J Clin Pathol. 2019;152(6):706-17. https://pubmed.ncbi.nlm.nih.gov/31355851 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6829017 https://doi.org/10.1093/ajcp/aqz089 DOI: https://doi.org/10.1093/ajcp/aqz089
Piva de Freitas P, Senna CG, Tabai M, Chone CT, Altemani A. Metastatic basal cell carcinoma: a rare manifestation of a common disease. Case Rep Med. 2017;2017:8929745. https://pubmed.ncbi.nlm.nih.gov/29279714 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5723960 https://doi.org/10.1155/2017/8929745 DOI: https://doi.org/10.1155/2017/8929745
Mills O, Thomas LB. Basaloid follicular hamartoma. Arch Pathol Lab Med. 2010;134(8):1215-9. https://pubmed.ncbi.nlm.nih.gov/20670146 https://doi.org/10.5858/2008-0620-RS.1 DOI: https://doi.org/10.5858/2008-0620-RS.1
Gupta B, Bhattacharyya A, Singh A, Sah K, Gupta V. Basaloid squamous cell carcinoma - A rare and aggressive variant of squamous cell carcinoma: a case report and review of literature. Natl J Maxillofac Surg. 2018;9(1):64-8. https://pubmed.ncbi.nlm.nih.gov/29937662 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5996643 https://doi.org/10.4103/njms.NJMS_14_17 DOI: https://doi.org/10.4103/njms.NJMS_14_17
Knackstedt T, Samie FH. Sebaceous carcinoma: a review of the scientific literature. Curr Treat Options Oncol. 2017;18(8):47. https://pubmed.ncbi.nlm.nih.gov/28681210 https://doi.org/10.1007/s11864-017-0490-0 DOI: https://doi.org/10.1007/s11864-017-0490-0
Del Marmol V, Lebbé C. New perspectives in Merkel cell carcinoma. Curr Opin Oncol. 2019;31(2):72-83. https://pubmed.ncbi.nlm.nih.gov/30694842 https://doi.org/10.1097/CCO.0000000000000508 DOI: https://doi.org/10.1097/CCO.0000000000000508
Lewis KD, Peris K, Sekulic A, et al. Final analysis of phase II results with cemiplimab in metastatic basal cell carcinoma after hedgehog pathway inhibitors. Ann Oncol. 2023;35(2):221-8. https://pubmed.ncbi.nlm.nih.gov/38072158 https://doi.org/10.1016/j.annonc.2023.10.123 DOI: https://doi.org/10.1016/j.annonc.2023.10.123
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Reynaldo Gabriel Paulino, Karen B. Damian, MD, FPSP, Clarisse Veronica L. Mirhan, RMT, MD, John Ricardo Chua, Erwin Gerard Geron

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.









 @philippinepathologyjournal
@philippinepathologyjournal