Lipomatous Angiomyofibroblastoma in the Vulva
A Case Report with Review of Literature
DOI:
https://doi.org/10.21141/PJP.2025.15Keywords:
vulva, angiomyofibroblastoma, lipomatous angiomyofibroblastomaAbstract
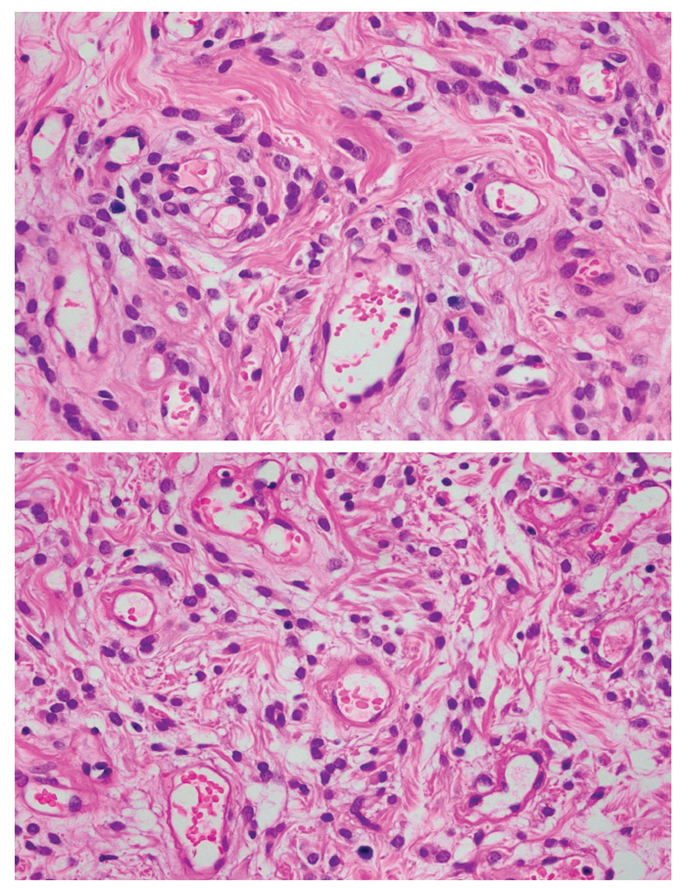
This is a case of a 55-year-old female, surgical menopause for nine years, not on hormone therapy with one year history of a progressively enlarging left vulvar mass, who sought consult and subsequently underwent excision of mass. Microscopic findings showed alternating hypo- and hypercellular areas composed of plump spindle to epithelioid cells distributed in an edematous stroma with varying amount of collagen. Tumor cells have bland chromatin, inconspicuous nucleoli, and absent mitoses. The cells surround small to medium-sized thin-walled, hyalinized vessels found in hypercellular areas. An adipocytic differentiation of more than fifty percent of tumor is observed further classifying this neoplasm as lipomatous angiomyofibroblastoma, making this an even rarer type of benign mesenchymal tumor of the vulva. Immunohistochemistry stains performed showed positive staining for vimentin, smooth muscle actin, BCL-2, ER, PR, and negative staining for desmin which supports the diagnosis. The clinical presentation, operative findings, histopathologic features and the various considerations are discussed. Literature review of vulvar angiomyofibroblastoma is also presented.
Downloads
References
Fletcher CD. Angiomyofibroblastoma. In: World Health Organization Classification of Soft Tissue and Bone Tumours. 5th ed. Lyon, France: International Agency for Research on Cancer; 2020.
Magro G, Righi A, Caltabiano R, Casorzo L, Michal M. Vulvovaginal angiomyofibroblastomas: morphologic, immunohistochemical, and fluorescence in situ hybridization analysis for deletion of 13q14 region. Hum Pathol. 2014;45(8):1647-55. https://pubmed.ncbi.nlm.nih.gov/24880711 https://doi.org/10.1016/j.humpath.2014.03.020 DOI: https://doi.org/10.1016/j.humpath.2014.03.020
Matsukuma S, Koga A, Suematsu R, Takeo H, Sato K. Lipomatous angiomyofibroblastoma of the vulva: A case report and review of literature. Mol Clin Oncology. 2016;6(1):83-8. https://pubmed.ncbi.nlm.nih.gov/28123735 https://pmc.ncbi.nlm.nih.gov/articles/PMC5245068 https://doi.org/10.3892/mco.2016.1078 DOI: https://doi.org/10.3892/mco.2016.1078
Guilmette J, Gauthier P, Rahimi K. Lipomatous angiomyofibroblastoma: a 20-year literature review. HumPathol: Case Rep. 2015;28(3):83-6. https://doi.org/10.1016/j.ehpc.2015.01.002 DOI: https://doi.org/10.1016/j.ehpc.2015.01.002
Abarzúa-Araya A, Lallas A, Piana S, Longo C, Moscarella E, Argenziano G. Superficial angiomyxoma of the skin. Dermatol Pract Concept. 2016;6(3):47-9. https://pubmed.ncbi.nlm.nih.gov/27648383 https://pmc.ncbi.nlm.nih.gov/articles/PMC5006552 https://doi.org/10.5826/dpc.0603a09 DOI: https://doi.org/10.5826/dpc.0603a09
Medeiros F, Erickson-Johnson M, Keeney G, et al. Frequency and characterization of HMGA2 and HMGA1 rearrangements in mesenchymal tumors of the lower genital tract. Genes Chromosomes Cancer. 2007;46(11):981-90. https://pubmed.ncbi.nlm.nih.gov/17654722 https://doi.org/10.1002/gcc.20483 DOI: https://doi.org/10.1002/gcc.20483
Nucci M, Fletcher C. Liposarcoma (atypical lipomatous tumors) of the vulva: a clinicopathologic study of six cases. Int J Gynecol Pathol. 1998;17(1):17-23. https://pubmed.ncbi.nlm.nih.gov/9475187 https://doi.org/10.1097/00004347-199801000-00004 DOI: https://doi.org/10.1097/00004347-199801000-00004
Romblon K, Poblete R. Angiomyofibroblastoma of the vulva: a diagnostic dilemma. Phil J Obstet Gynecol. 2018;42(3):30-6. Herdin ID: 102490-22031706405143
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Clarisse Young, Agustina Abelardo

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.









 @philippinepathologyjournal
@philippinepathologyjournal